
Pneumococcal Conjugate Vaccines

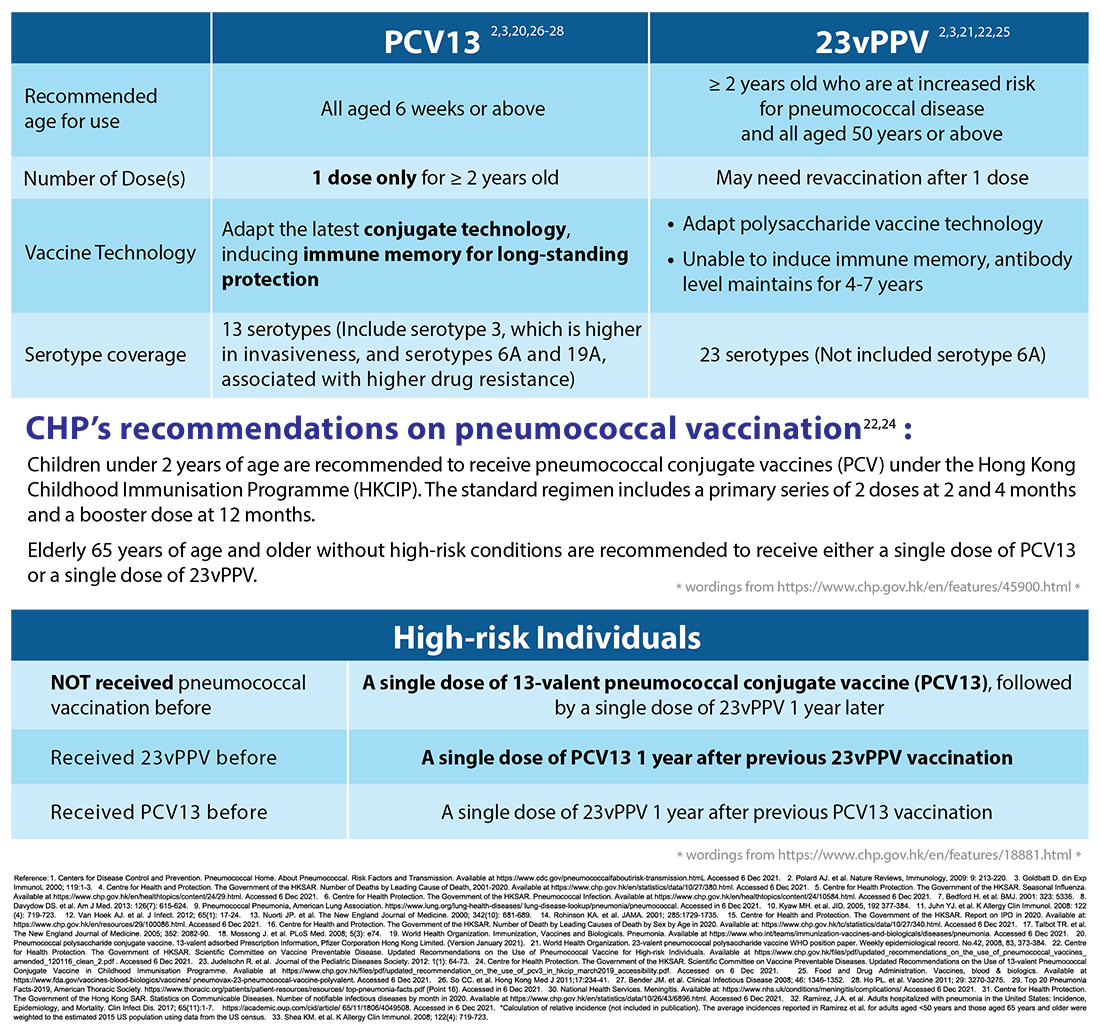
Sourse:Pfizer (last update Apr 2022)




HOME | About Us | Health Check | Vaccination | Other Service | Privacy Policy | Contact Us | Sitemap | Recruit
HOME | About Us | Health Check | Vaccination | Other Service
Privacy Policy | Contact Us | Sitemap | Recruit
Copyright © 2018 毅力醫護健康集團 Kinetics Medical & Health Group 版權所有 不得轉載
